Psoriatic arthritis is a type of inflammation arthritis mostly found in people who have psoriasis (a skin disease). About 10% to 30% of people with psoriasis get PsA (psoriatic arthritis). This condition affects both genders in equal numbers. It also usually appears in people who are between 20 and 50 years of age. Unfortunately, PsA does not have a cure. However, if it is caught early and the appropriate treatment given, there is a high likelihood that you will be able to take control of the disease and prevent severe joint damage.
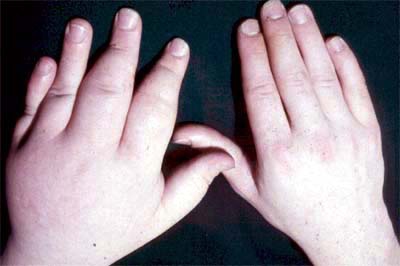
What Is Psoriatic Arthritis?
Psoriasis is a disease whereby white and red patches develop on your skin. It is caused when the immune system starts attacking the skin. People who have psoriasis also get psoriatic arthritis when the immune system attacks the joints resulting in inflammation. Just like psoriasis, PsA symptoms subside and flare to varying degrees from one person to the other. The symptoms even change location in one body over some time.
Types of Psoriatic Arthritis
Below are the five different types of psoriasis arthritis:
Arthritis mutilans: This is a destructive, deforming and severe form of psoriatic arthritis. It primarily affects small joints like those found in the toes and fingers, close to nails.
Spondylitis: This is a condition that affects your spinal column. It may cause stiffness and inflammation in the pelvic area (sacroiliac region), spinal vertebrae, lower back or neck. Making motions is also difficult.
Distal interphalangeal predominant (DIP): DIP psiriatic arthritis primarily involves small joints like those found in the toes and fingers.
Asymmetric psoriatic arthritis: This type of PsA involves 1 to 3 joints, small or large, in the body. For example, all or one joint of the fingers, the hip or knee
Symmetric PsA: This psoriasis affects the same joints - normally in multiple and matching pairs and on opposite sides of the body.
What Are the Symptoms of Psoriatic Arthritis?
Psoriasis and PsA are chronic and get worse over time. There are, however, some periods when the symptoms go into remission or improve and other times when they get worse. PsA can affect joints in one or both sides of the body. The symptoms and signs of PsA often resemble those of rheumatoid arthritis. Both types of arthritis make the joints painful, warm and swollen to the touch.
PsA is also likely to cause:
Lower back pain: Some people who have PsA develop spondylitis – A condition that causes joints inflammation – these are the joints between the pelvis and spine and spine vertebrae.
Foot pain: PsA can also cause pain where the ligaments and tendons attach to the bones. More so, at the sole of the foot or back of your heel.
Swollen toes and fingers: PsA can cause sausage-like swelling of the fingers, which is also quite painful. Deformities and swelling may also develop in your feet and hands prior to major joints symptoms.
When to See a Doctor
Make sure you consult your doctor about any joint pain especially if you have psoriasis. PsA can develop suddenly or slowly. Either way, if it goes untreated, your joints can be severely damaged.
What Are the Causes & Risk Factors of Psoriatic Arthritis?
The exact cause of PsA remains unknown. The affected joint’s synovium (tissue that surrounds joints) gets inflamed as well as other body parts like the ligaments and tendons. The following are some of the factors that can trigger PsA:
| Risk Factors | Description |
| Injury to the skin | Skin injury has been linked to plaque psoriasis. For instance, excessive scratching or skin inflammation can cause psoriasis. |
| Drugs | There are several medications that can aggravate psoriasis. For example, Antimalarials, Beta-blockers and Lithium. |
| Hormone changes | Psoriasis severity can fluctuate when there is change in hormones. These diseases peak when a woman is hitting menopause and puberty. Pregnant women also have hormone changes that can improve the symptoms. On the other hand, the symptoms will likely flare after they has given birth, if there are any changes. |
| Alcohol | Alcohol is a risk factor to middle-aged men for psoriasis. |
| Smoking | Smokers are at high risk of getting chronic plaque psoriasis. |
| Emotional stress | In many cases, psoriasis increases when a person has emotional stress. |
| HIV | Psoriasis worsens after a person gets infected with HIV. It is, however, less active in advanced HIV infection. |
| Streptococcal infections | There is some evidence that suggests that these types of infections cans cause plaque psoriasis. It is a psoriasis that resembles small drops that are red in color on the skin. |
| Sunlight | While some people find sunlight to help with psoriasis, there are a small number of people who find that sunlight worsens their symptoms. Sunburns can also worsen the psoriasis. |
What Are the Treatments for Psoriatic Arthritis?
Psoriasis arthritis does not have a cure. As such, its treatment focuses on inflammation control in the affected joints, thereby preventing joint disability and pain. Here are some of the drugs that are used to treat psoriasis arthritis:
TNF-alpha inhibitors: These help to reduce swollen or tender joints, morning stiffness and pain. Examples include certolizumab (Cimzia), golimumab (Simponi), adalimumab (Humira), infliximab (Remicade) and etanercept (Enbrel).
Immunosuppressants: These tame the immune system, which is normally out of control in psoriasis arthritis. Examples of immunosuppressants include cyclosporine (Gengraf, Neoral, Sandimmune) and azathioprine (Imuran, Azasan).
Disease-modifying antirheumatic drugs (DMARDs): These are used to slow down psoriatic arthritis progression. They save tissues and joints from permanent harm. They include sulfasalazine (Azulfidine), leflunomide (Arava) and methotrexate (Trexall).
NSAIDs: These help reduce inflammation and relieve pain. Over-the-counter NSAIDs include naproxen sodium (Aleve) and ibuprofen (Advil, Motrin IB).
Other treatments include:
Joint replacement surgery: If psoriatic arthritis severely damages your joints, they can be replaced with artificial prostheses that have been made of plastic and metal.
Steroid injections: Steroids help reduce inflammation fast. They are sometimes injected into the affected joint.
Home Remedies
Pace yourself: Battling inflammation and pain can leave you exhausted. Arthritis medications can also cause fatigue. Therefore, find ways of relaxing during the day-breaks even if you are working.
Use hot and cold packs: Cold packs help to numb the pain sensation. Hot packs will help relieve pain and relax tense muscles.
Exercise regularly : This helps to keep the joints flexible and muscles strong. Try less stressful exercises like walking, swimming and biking.
Maintain healthy weight: This will help put less strain on your joints. As a result, you will have less pain and increased mobility and energy. Eat more whole grains, vegetables and fruits.
Protect the joints: Do not strain finger joints when carrying heavy bags. Instead, use jar openers to open cans and backpacks. Push doors open using your whole body and not the fingers only.

View All Comments /Add Comment