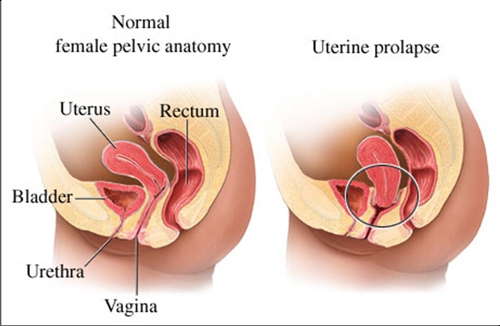
Prolapsed uterus is a condition characterized by weak pelvic muscles and ligaments that fail to support the uterus. This usually leads to uterine prolapsed – it means your uterus has sagged down into your vagina. This condition can be divided into two categories – it may be complete prolapse or incomplete. If it is complete prolapse, the tissue becomes visible outside the vagina. Some medical professionals divide the condition into four stages instead of two categories. This includes:
Stage I – if your uterus goes to the upper half of your vagina.
Stage II – if your uterus has come close to the opening of your vagina.
Stage III – if your uterus comes out of your vagina.
Stage IV – if uterus has come out of vagina (uterus falling out completely).
It is therefore important to get in touch with your healthcare provider if you notice specific symptoms related to this condition.
What Are the Symptoms of a Prolapsed Uterus?
Symptoms of the prolapsed uterus include:
Feeling as if you are sitting on a ball
A pulling sensation in your pelvis
Urinary leakage or retention
Trouble having a bowel movement
Lower back pain
Trouble having intercourse
If you have any of these symptoms, it is time to see your doctor. If caught early, it can be treated with remedies that do not require surgery.
What Causes a Prolapsed Uterus?
There are several possible causes of uterine prolapse. The most common cause is the loss of estrogen as a woman ages, causing the weakening of the muscles in the pelvis that hold the uterus in place. Another cause is being overweight, which causes strain on the pelvis as it does with most of the body. Heavy lifting can also cause the prolapsed uterus.
Other causes include multiple childbirths or a difficult childbirth, chronic coughing such as having a bout with bronchitis, pneumonia or asthma, constipation or perhaps trauma to the pelvic area.
How Is Prolapsed Uterus Diagnosed?
Your doctor will conduct a physical exam to confirm if your symptoms are related to prolapsed uterus or it's something else.
Usually, your doctor will make you cough for added pressure on your abdomen. In certain cases, especially when you have ureteral obstruction, your healthcare provider may suggest a renal sonography or intravenous pyelogram (IVP), which involves injecting a dye into your vein and then taking x-rays to determine the severity of the situation. Sometimes, your doctor will recommend ultrasound to confirm there are no other serious pelvic issues causing certain symptoms.
How Is Prolapsed Uterus Treated?
Vaginal Pessary
Your doctor will insert this device into your vagina to keep your uterus in place. It is usually a temporary treatment, but you can discuss with your doctor to stick with it on a rather long-term basis. Vaginal pessaries are available in different sizes and shapes, so it is important that you work with a professional who could select the right device, considering the size of your vagina. It is equally important to learn how you can insert or remove the device on your own to limit clinical visits. Remember, the treatment option isn't for you if you're a patient of severe uterine prolapse.
Surgery
You may have to go for a surgery if you have weak or damaged pelvic floor tissues. Depending upon your condition, your surgeon may choose to perform a procedure through your vagina or suggest an abdominal surgery. The procedure usually involves grafting donor tissue or your own tissue – your surgeon may consider using synthetic material as well to provide support to your pelvic organs. You may be a good candidate of minimally invasive surgery that only requires smaller abdominal incisions with the help of surgical instruments. Sometimes, the only option is to remove your uterus through a surgical procedure. You should consider having your uterus removed if you're not planning future pregnancies; otherwise, you should consider repairing uterine prolapse. Whatever the procedure, be sure to discuss risk factors and other complications before you take the plunge.
Kegel Exercises
If your pelvic floor muscles aren't that weak, you may consider doing kegel exercises for improved strength. These exercises support your bladder, uterus and bowel. With a stronger pelvic floor, it becomes easier to provide support to your pelvic organs and cure prolapsed uterus. Keep the following things in mind when doing kegel exercises:
Exercise your pelvic floor muscles – the muscles you use to stop urinating – by tightening or contracting them.
Maintain the contraction for up to five seconds and then relax. Repeat the process after a break of five seconds.
Try to hold the contraction for about 10 seconds at a time.
Do at least three sets daily with 10 reps in each set.
It looks simple, but it's usually quite confusing for most women when they start for the first time. You may consider getting in touch with a physical therapist to learn which muscles to use while performing kegel exercises. The following video will help clear your doubts about prolapsed uterus and kegel exercises.
Other Remedies
Kegel exercises will definitely help, but you can take some other self-care measures to improve things quickly. Here are some tips that will help with your uterine prolapse:
Add high-fiber foods in your diet to prevent constipation.
Drink plenty of water and fluids to stay hydrated.
Don't life heavy weights and avoid straining.
Do what you can to control coughing.
Consider shedding off some pounds if you're obese.

View All Comments /Add Comment